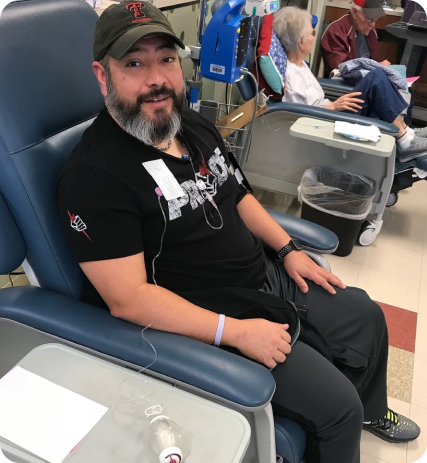
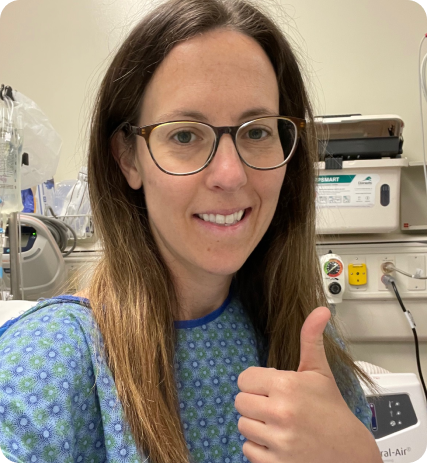
I received the grim diagnosis of Stage IV stomach cancer in 2017 at age 39. Doctors in Midland, Texas, where I was living at the time, told me the prognosis for metastatic stomach cancer was not good, with a five-year life expectancy of less than five percent and a treatment plan that they hoped would prolong–but not likely save–my life. Though I didn’t realize it until recently, the treatment I have been receiving since diagnosis correlates with my testing positive for the HER2 biomarker. I now believe the fact that I tested HER2+ and continue to receive treatment that targets my specific cancer type is a big part of why I’ll soon mark seven years as a stomach cancer survivor.
Diagnosis and Early Treatment
While I struggled with acid reflux for some time prior to my diagnosis, it was my only symptom and antacids seemed to help. I trained for months to run a half marathon in early December 2016, and had no problems during the race. However, upon returning to my engineering job after the holidays, I noticed I became short of breath climbing the stairs to my office. At first I chalked it up to intense training followed by holiday celebrations, but it progressed to the point where I would get winded walking down the hallway.
Concerned, I sought input from my primary care doctor. He ran many tests, and referred me to a specialist after seeing something on my lung X-ray. It took a while to get in with that doctor, who initially thought I may have COPD, but a lung biopsy in April 2017 revealed I had adenocarcinoma. At first, I thought that meant I had lung cancer, but my surgeon and oncologist explained that an endoscopy showed that my cancer had started in my stomach and metastasized to my lung.
Being generally healthy, it came as quite a shock that I had Stage IV stomach cancer, and I decided to get a second opinion on treatment at MD Anderson Cancer. As it turned out, the broad strokes of my diagnosis didn’t change much, and my early treatment plan involved a FolFOX chemotherapy infusion every two weeks for about seven months. Concurrently, since I was HER2+, I also began receiving Herceptin, a monoclonal antibody which specifically targets and binds to HER2 receptors in some cancer cells. While I haven’t had chemotherapy since 2017, I never stopped taking Herceptin, and will continue the protocol indefinitely.
The Case for Biomarker Testing
The only reason I was given Herceptin is my HER2 biomarker status. As my doctor explained it, I have an overexpression of the HER2 protein which can aids cancer cells to grow and divide. Herceptin interferes with that process and helps keep my cancer at bay. If my doctors hadn’t tested for the HER2 biomarker, I would never have received Herceptin at all. But they did test, I have been receiving Herceptin all along, and my scans since ending chemo have remained steady for almost seven years.
I will receive Herceptin every two weeks for the rest of my life. The chronic nature of this diagnosis and treatment can be tough–sometimes mentally more than physically. But, there’s so much to be hopeful about, and I would encourage newly-diagnosed stomach cancer patients to stay positive, talk with others going through similar struggles, ask their oncologist what biomarkers may impact their situation or give them a second line of treatment, and to try and think things through objectively.
In April 2024, I’ll mark seven years living with a stomach cancer diagnosis. It’s still hard to get used to at times, but I try to stay positive and control what I can, including my mindset around receiving treatment.