Test Your Biomarkers

Why Biomarkers?
Before beginning a treatment plan, it's important to ask about biomarkers. Biomarkers can help you understand what your tumor is made of, and they can also let you know what treatments you may qualify for or which treatments are unlikely to work. Many clinical trials are designed around biomarkers. Biomarkers are the backbone of personalized medicine.
Biomarker Basics
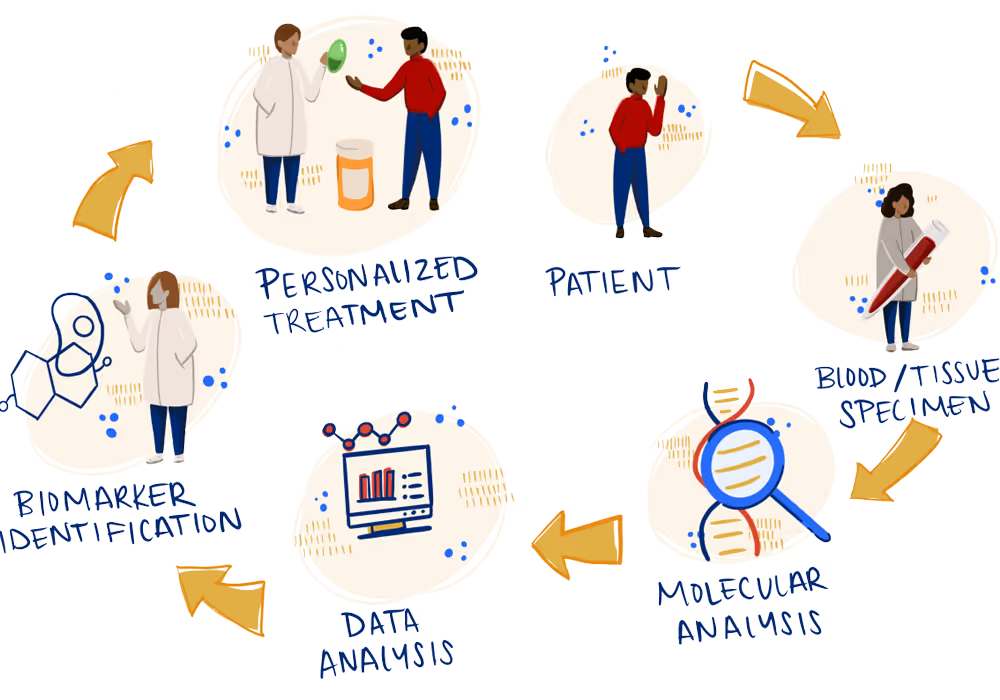
Biomarkers are bits of information unique to you and your cancer. If you look deep inside a tumor, you’ll find that it’s made up of all sorts of genes and proteins. Some of them are acting normal and healthy; others are not. Biomarker testing uncovers which genes and proteins led to your cancer. Precision medicine is the emerging field of cancer treatment where certain biomarkers can be targeted with specific drugs.
A doctor (sometimes a surgeon, but usually an oncologist) should order biomarker testing. Your doctor should help you understand your biomarker results and how they impact your treatment plan. All cancer patients need biomarker testing, but not all patients need the same biomarker tests. Biomarker testing is still relatively new. If your doctor doesn’t mention it, ask!
Biomarker testing can be performed on solid tissue biopsy and/or blood (which is called liquid biopsy). Traditional biomarker tests look for a single gene, new Next Generation Sequencing (NGS) tests look for multiple biomarkers in a single test. The biomarker testing you receive will depend on cancer guidelines for your type of cancer and your stage.
Biomarkers give critical information about your cancer. Some biomarkers can predict if your cancer will or won’t respond to certain drugs. Others offer a picture into how aggressive or mild your cancer is. Gone are the days where every advanced cancer is treated with the exact same protocols. Biomarker testing will allow your team to understand the unique makeup of your cancer and build a unique, individual treatment plan.
Test for biomarkers as soon as treatment conversations begin. Ideally, you will have biomarker test results before you begin any treatment (including surgery in some cases). Not all cancers have the same biomarkers, and certain drugs are available only for patients with specific biomarkers. Your doctor may request additional or repeat biomarker tests as you progress throughout your treatment.


Test first. Test early. The best treatment for your cancer is personal.

Biomarkers are the backbone of personalized medicine.
Clinical Trials
Most clinical trials exploring new cancer drugs will require biomarker testing. Clinical trials are where up-and-coming biomarkers become star players, where experimental approaches to treating a cancer become the standard-of-care. Clinical trials are truly the future of medicine. There are clinical trials available for patients of every GI cancer type and nearly every biomarker.
Biomarkers and biomarker testing
Many common insurers cover the cost of most biomarker testing. Liquid biopsies may be an exception. Patient financial assistance (Patient Assistance Programs) may be available. Check with your healthcare provider and insurance company to learn more.
A lot of patients get genetic testing and biomarker testing confused. Genetic testing is ordered by a genetic counselor/geneticist and looks for germline mutations. These are gene mutations you’re born with that may have caused your cancer. Biomarker testing looks for somatic mutations, or problems in your genes/proteins that occurred after you were born. Biomarker testing and genetic testing have complementary roles when it comes to understanding why your cancer formed, but they are different tests.
You can still have biomarker testing even if you’ve received treatment. Start the conversation with your doctor if you’re unsure. If you’re on a targeted therapy or immunotherapy, it’s likely you did receive testing, but ask to see your results. If there aren’t any, request the test.