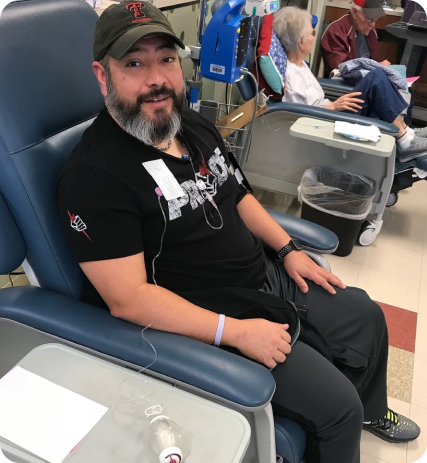
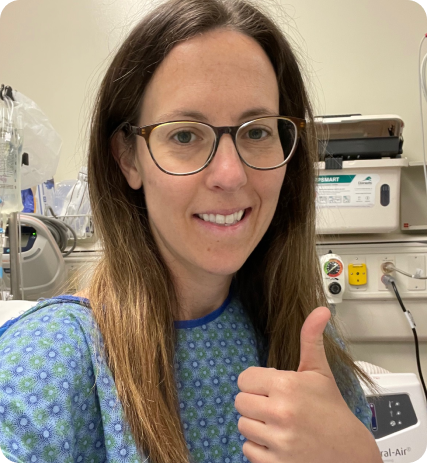
In late September of 2021, I was diagnosed with Stage IV stomach cancer. I had just turned 50, and was enjoying my full, active life as a mother of teen girls and successful esthetician. Although many of my family members have died from cancer, it came as a shock that my disease had already metastasized to my bones and lymph nodes. Surgery was not an option for me since my cancer had already spread, but I was tested for HER-2 and PD-L1, the two known biomarkers at that time. I had a PD-L1 score of 10, which meant I “qualified” for immunotherapy.
Diagnosis and Early Treatment
Prior to the Covid-19 pandemic, I suffered from stomach pain and dysphasia, but didn’t seek care until those symptoms intensified and I developed such severe pain in my arm and shoulder that I couldn’t lift my right arm.
In April 2022, an endoscopy showed that my stomach tumor was completely gone, an outcome my doctor said was “a miracle.” I stayed on Opdivo, but stopped taking FOLFOX after six rounds, because it left me so battered that my doctor no longer recommended it. Instead, I switched to a lower-dose chemo and by late 2022, my APL was at 58–within the normal range. In April 2023, my doctors said, while I would need to be on immunotherapy indefinitely, I had what was known as a “complete clinical response” and I decided to give my body a break from chemo.
The Case for Biomarker Testing
Unfortunately, in the fall of 2023, my APL was again elevated. I am continuing with my Opdivo-chemo-Xgeva regimen, and I also underwent cyberknife radiation to target two cancerous areas in my spine. Many people with Stage 4 stomach cancer don’t live as long as I already have, and I believe that my PD-LI biomarker and Opdivo treatment have been instrumental in keeping my cancer manageable for the past two years. I am grateful for that, but I can’t help but wonder what other treatments might be available to me if I’d known sooner about biomarkers.
In August 2022, there was a lot of excitement about a new biomarker called MSI-high. However, I could not accurately be tested for it through the now-standard liquid biopsy, because my initial treatment had done such a great job eradicating my stomach tumor that there was no Circulating Tumor DNA (ctDNA) in my blood. In hindsight, I wish my insurer had covered more thorough testing and a much larger sample of my stomach tumor to be saved, because understanding of biomarkers, new treatments and genetics are evolving and developing so rapidly.
The world of stomach cancer treatment has changed dramatically since my initial diagnosis just two years ago. In addition, I recently learned that I have a pathogenic variant on my CTNNA1 gene that is correlated with stomach cancer. My sister and both of my daughters also have the variant, and are facing battles of their own. We don’t yet know how this might affect treatment down the road.
Today, I am advocating for biomarker testing in part because I believe targeted treatment can impact stomach cancer outcomes, in part because it benefits me to stay connected with the stomach cancer community, and in part because I want my girls, and all newly-diagnosed patients to understand the importance of early biomarker testing, prior to treatment. The more someone understands about their specific cancer, the more treatment options they may have in the present and, importantly, in the future.